
Your Wheelchair Guide: Reduce Pressure Sores on the Buttocks from Sitting
Pressure injuries can be a significant issue for wheelchair users, but technologies exist to help prevent them.
For people with high-risk factors, pressure injuries can present significant challenges—particularly when their lifestyle or health condition makes them chronically vulnerable to developing a sore. Wheelchair users are among this group.
Pressure sores are caused by elevated, sustained pressure on the skin. As the sore develops, a warm, red, spongy area becomes apparent, which can quickly lead to a break in the skin’s physical surface. Reduced blood flow to the area may lead to dead tissue and further injury. When not managed quickly, pressure injuries will result in serious skin damage, and sometimes even death.
For those who sit in wheelchairs, a pressure injury can develop very quickly— especially on the buttocks, which experiences the most pressure. Fortunately, there are certain lifestyle changes and technological additions that can help to reduce pressure sores on the buttocks from sitting.
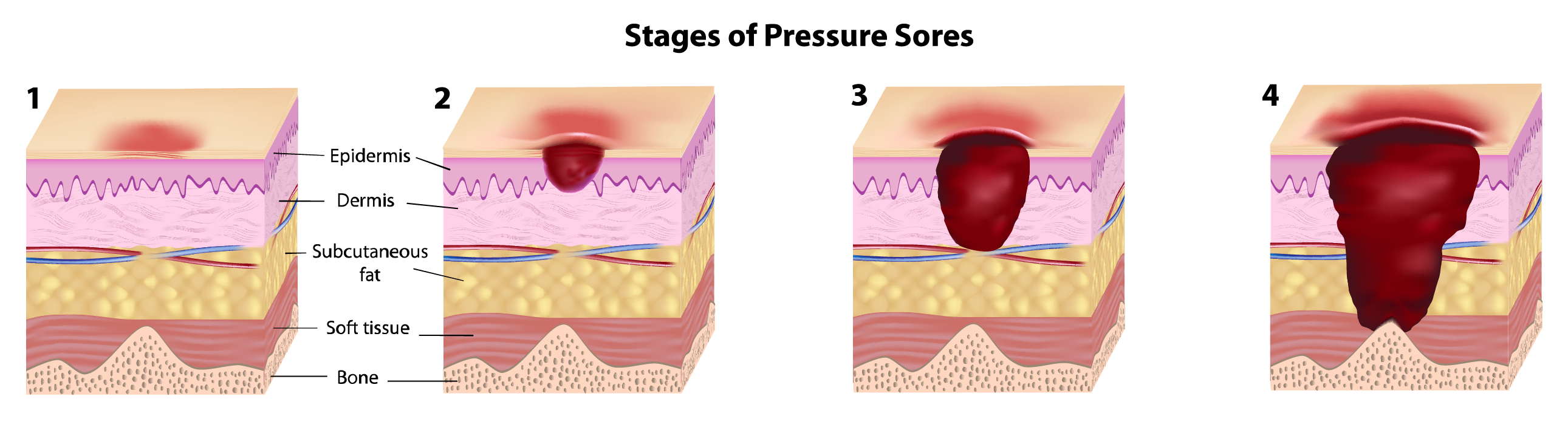
Pressure Sores: The 4 Stages of Pressure Sores
Understanding how pressure injuries develop is key to preventing and mitigating them. The National Pressure Ulcer Advisory Panel describes the four stages of pressure injury development as follows.
Stage I – Non‐blanchable Erythema: "Intact skin with non‐blanchable redness of a localized area usually over a bony prominence. Darkly pigmented skin may not have visible blanching; its color may differ from the surrounding area. The area may be painful, firm, soft, warmer or cooler as compared to adjacent tissue. Category I may be difficult to detect in individuals with dark skin tones. May indicate ‘at risk’ persons."
Stage 2 – Partial Thickness: "Partial thickness loss of dermis presenting as a shallow open ulcer with a red pink wound bed, without slough [dead tissue]. May also present as an intact or open/ruptured serum‐filled or sero‐sanguinous [serum and blood] filled blister. Presents as a shiny or dry shallow ulcer without slough or bruising [bruising indicates deep tissue injury]. This category should not be used to describe skin tears, tape burns, incontinence associated dermatitis, maceration [damage through the skin being wet] or excoriation [damage through scratching/abrasion or burns]."
Stage 3 – Full Thickness Skin Loss: "Full thickness tissue loss. Subcutaneous fat may be visible but bone, tendon or muscle are not exposed. Slough may be present but does not obscure the depth of tissue loss. May include undermining and tunnelling. The depth of a Category/Stage III pressure ulcer varies by anatomical location. The bridge of the nose, ear, occiput [back of the head] and malleolus [ankle] do not have [adipose] subcutaneous tissue and Category/Stage III ulcers can be shallow. In contrast, areas of significant adiposity can develop extremely deep Category/Stage III pressure ulcers. Bone/tendon is not visible or directly palpable."
Stage 4 – Full Thickness Tissue Loss: "Full thickness tissue loss with exposed bone, tendon or muscle. Slough or eschar [scabbing] may be present. Often includes undermining and tunnelling. The depth of a Category/Stage IV pressure ulcer varies by anatomical location. The bridge of the nose, ear, occiput and malleolus do not have [adipose] subcutaneous tissue and these ulcers can be shallow. Category/Stage IV ulcers can extend into muscle and/or supporting structures (e.g. fascia, tendon or joint capsule) making osteomyelitis [bone infection] or osteitis [inflammation of bone] likely to occur. Exposed bone/muscle is visible or directly palpable."
Practices for Reducing Pressure Sores on Buttocks
When a person spends a lot of time sitting in a wheelchair, they are more susceptible to developing injury—especially on an area of intense pressure like the buttocks. However, those sitting in wheelchairs can also develop pressure sores on the backs of their thighs, their lower back and the folds of their knees. Certain practices can help to reduce injuries from occurring.
Keep skin clean and dry: Moist skin creates an atmosphere where a sore can develop quickly, so keeping the skin dry when in a wheelchair can help. Regular bathing is another important preventive skin care measure, as bacteria increases the risk of infection in a developing sore.
Implement softer seating: Sitting in a wheelchair consistently can become uncomfortable, and excess pressure increases the risk of developing a pressure injury on the buttocks. Consider adding a seat cushion or gel cover to the wheelchair seat to soften the surface and help relieve the pressure.
Reposition consistently: Oftentimes, those in wheelchairs are partially immobile — but that doesn’t mean movement isn’t possible. Whether by implementing a repositioning schedule or intentionally getting out of the chair when possible, consistent repositioning is essential for relieving pressure.
Put feet on ground to redistribute pressure: Proper adjustment of footrest is crucial to safe seating and managing pressure. By placing the feet on the ground or on the wheelchair footrest, shear can be prevented, which reduces the opportunity for an injury to develop. In addition, moving the feet can take pressure off high-pressure areas, and even the low back.
Use pressure mapping: Pressure mapping technology uses sensors to provide continuous data on the affected areas. Seat cushions equipped with pressure mapping can help wheelchair users and their health professionals to make informed decisions for repositioning to proactively prevent a sore from developing.
Can pressure mapping help to reduce pressure sores on buttocks from sitting?
Technologies are available that help to identify pressure injuries and prevent their development, and pressure mapping is an excellent option.
Using sensors, pressure mapping systems provide more detailed information than a physical exam could reveal, making it possible to monitor patients at high risk for injury such as wheelchair users.
Pressure mapping provides live information, showing points on a patient’s skin that are under particularly high pressure, or below-optimal pressure. Armed with continuous data, health professionals and wheelchair users themselves can actively work to redistribute pressure as needed (and not where it isn’t).
Using this technology, clinicians are equipped to run interference on high-risk areas, allowing patients to stay healthy and painless while maximizing efficiency in a healthcare setting.
XSENSOR’s Wheelchair Pressure Mapping System
Wheelchair users continue to experience a higher number of pressure injuries—despite how wheelchairs and cushions have continued to adapt and improve over time.
At XSENSOR, we’ve combined global innovation with scientific expertise to create interface pressure management technologies that help to measure pressure points and provide the most benefit when used proactively. By working to mitigate and prevent pressure development, we enable healthcare professionals to provide preventative care and patients to live more comfortable, healthy lives in their wheelchairs.
Our advanced pressure imaging system for wheelchair seating—ForeSite SS—is the market leader. This technology is medically certified but also requires minimal training, which makes it ideal for busy medical professionals and their patients.
Combining top-tier sensor accuracy and clear, high-resolution images with smart, easy-to-use software, the ForeSite SS system helps clinicians ensure their clients have comfortable and effective wheelchair seating that also monitors skin pressure. This helps to prevent sores from developing, alleviates painful, dangerous injuries and ultimately offers better patient care for wheelchair patients.


