
How to Prevent Pressure Sores in Hospitals
XSENSOR Technology helps to mitigate pressure sore risks.
When it comes to hospital stays—especially extended stays—the topic of pressure injuries is more relevant than any hospital administrator would like. Pressure sores and pressure ulcers are intensely common, with over 2.5 million patients in the United States developing hospital acquired pressure ulcers (HAPUs), and an unfortunate 60,000 pressure sore-induced deaths or injuries annually.
So how can we work to mitigate their risk and improve patient outcomes? By continuously monitoring skin, keeping an eye on areas of high pressure, and working to predict spots that are vulnerable to developing sores in the first place.
At XSENSOR, we’ve developed software and sensors that equip healthcare workers to make informed decisions that help prevent pressure ulcers. Our guide to preventing pressure sores in hospitals is the first step to increasing risk assessment abilities and preventing pressure ulcers for your patients.
How to Prevent Pressure Sores in Hospitals
Preventing pressure ulcers in hospitals can be done, but it requires special attention and resources: continuous skin monitoring to identify problem areas, and the implementation of specialized equipment that helps medical staff create proper treatment plans for their patients. XSENSOR’s Intelligent Dynamic Sensing technology is built for this purpose—to help clinicians reduce the risk of pressure injuries from the beginning of any hospital stay.
It’s essential to understand how pressure sores develop and how hospitals can identify risks in order to prevent them with high success levels.
Hospital directors focused on upping patient safety, comfort and health: here’s what you need to know.

Early Signs of a Pressure Sore
Pressure ulcers are significant for anyone who develops them, but we know certain patients are at greater risk. And while the early signs of pressure sores are known to most medical professionals, creating risk assessment plans for high-risk patients is key to prevention or catching pressure sores early.
With XSENSOR’s medical technology, healthcare workers can predict pressure ulcer locations and monitor risk of sore development before it even begins. Without this technology, healthcare workers often left to work on reversing damage once it’s begun — when the skin has already started to redden, inflame and weaken.
Pressure Sores: The 4 Stages
For patients who develop pressure ulcers in a hospital bed, there are four main stages of injury to the skin. Whatever the stage, it’s important to manage them immediately with strategies and technology that prevent further development.
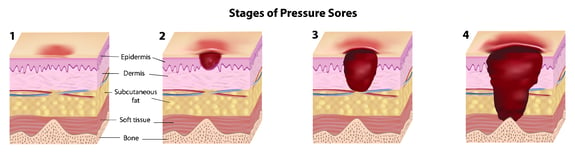
Here are the four stages of pressure sores, from early skin damage to serious ulcer progression:
Stage 1 Pressure Injuries: Early on in ulcer development, the skin is developing injury. While no open sores or broken skin are present yet, skin may appear redder, warmer or firmer than usual. Known as a non-blanchable erythema of intact skin, the color change may even indicate the beginnings of a serious injury to the deep tissue.
Stage 2 Pressure Injuries: Here is where the true sore, or ulcer, develops as a break in the skin. This is often very painful, and can create serious damage within the skin. Known as partial-thickness skin loss with exposed dermis, these bed wounds can quickly become something worse.
Stage 3 Pressure Injuries: In this stage, the pressure ulcer has traveled into the soft tissue beneath the skin. Known as full-thickness skin loss, this pressure sore stage may showcase a deep wound, especially in an area with more adipose tissue.
Stage 4 Pressure Injuries: By the final and most serious stage of a pressure sore, the skin may have receded into the muscle tissue or the bone, causing lasting damage to the skin and underlying areas. Known as full-thickness skin and tissue loss, this stage can mean visible or palpable fascia, bone, muscle or tendon.
The Implications of Pressure Injuries
It’s no secret that pressure injuries can become incredibly serious, from deep tissue damage all the way to sepsis, resulting in death. Developing pressure sores can lead to skin damage and infection, causing injuries that are, in many cases, preventable. They also place a significant legal strain on hospitals. According to the Agency for Healthcare Research and Quality, there are more than 17,000 lawsuits filed related to pressure ulcers a year, and the pressure ulcers themselves cost between $9.1 billion and $11.6 billion a year in fees.
With unnecessary patient suffering and legal issues both at stake, it’s important to create a culture of urgency within hospitals to reduce pressure sore cases among patients. By becoming quickly aware of the issues and monitoring skin from the beginning, this is much easier to do.
Equipment for Relieving Pressure Sores
XSENSOR’s Continuous Skin Monitoring (CSM) technology is specifically geared towards helping clinicians effectively position patients to prevent dangerous pressure exposure (or elevated pressure). By integrating hospital equipment that monitors patient skin and predicts problem areas from the outset of the stay, it’s much easier to mitigate risks and stop pressure sores before they start.
Where it Starts: The Hospital Bed
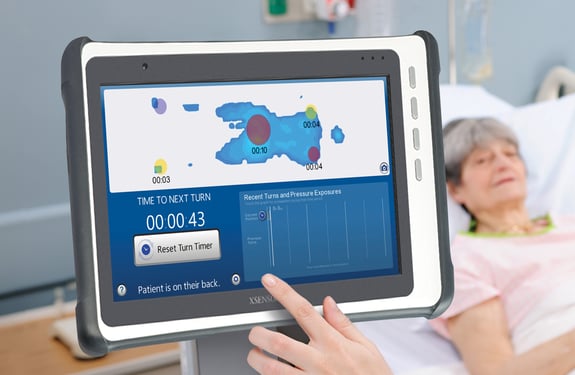
When preventing pressure sores in hospitals, hospital beds themselves are determining factors. This is where XSENSOR’s ForeSite Intelligent Surface (IS) system comes in.
The system works using either a mattress overlay or an integrated mattress for hospital beds, embedded with thousands of sensor cells that continuously monitor patient body surface pressures. A bedside monitor displays real-time pressure images and clearly identifies parts of the body under sustained elevated pressure. A turn clock tracks the time between patient repositioning, and alerts staff to adjust their rotation.
This, ultimately, leads to every medical professional’s goal: quality patient care and positive patient outcomes. With the support of XSENSOR’s technology, medical staff can focus on patient care where it is most needed, putting their energy into essential clinical activities, and not into preventative efforts that are unnecessary (or ineffective)—such as waking sleeping patients to rotate them, if they aren’t truly at risk of developing pressure sores.
Through providing caregivers with consistent information, XSENSOR’s ForeSite IS increases the integrity in continuity of care, helps avoid pressure ulcers from forming and may improve healing time for existing wounds to also reduce the length of hospital stays due to pressure ulcers.
The system comes with:
- An intelligent mattress overlay or an integrated mattress sensor
- 1,600 sensing points that cover a large surface area of skin
- A bedside monitor
- A disinfectable cover
Beyond improved patient outcomes, implementing this technology will improve the workload on medical staff. Equipped with insights on their patients’ skin conditions, staff will be freed up to shift their attention to demanding issues—a particularly relevant concern in light of COVID-19. Lower incidence of pressure ulcers will also lessen the load of ulcer-related patient care and administrative reporting.
In short, XSENSOR’s pressure monitoring technology is key in creating a more progressive, healthy hospital culture—one where patient outcomes (seen through the prevention of pressure sores) are positive, where staff workloads are well-managed and where medical professionals are equipped to make sound decisions. XSENSOR’s ForeSite IS should be considered by hospital administrators as an essential piece of equipment.
When choosing equipment that will consistently improve patient care, XSENSOR’s technology is indispensable. With careful designs geared specifically toward patient comfort and health, XSENSOR’s pressure sensing technology is key to preventing debilitating pressure sores in hospitals.
By improving risk assessment with XSENSOR equipment, healthcare workers are empowered to prevent pressure ulcers before they begin, saving patients from unnecessary suffering and hospitalization, and freeing up staff to focus their attention where it is most needed.

